Neuropathy is a condition in which the nerves in the body become damaged from a number of different illnesses. Nerves from any part of the body, including the foot, can be damaged. There are several forms of neuropathy including peripheral neuropathy, cranial neuropathy, focal neuropathy, and autonomic neuropathy. Furthermore there is also mononeuropathy and polyneuropathy. Mononeuropathies affect one nerve while polyneuropathies affect several nerves. Causes of neuropathy include physical injury, diseases, cancers, infections, diabetes, toxic substances, and disorders. It is peripheral neuropathy that affects the feet.
The symptoms of neuropathy vary greatly and can be minor such as numbness, sensation loss, prickling, and tingling sensations. More painful symptoms include throbbing, burning, freezing, and sharp pains. The most severe symptoms can be muscle weakness/paralysis, problems with coordination, and falling.
Podiatrists rely upon a full medical history and a neurological examination to diagnose peripheral neuropathy in the foot. More tests that may be used include nerve function tests to test nerve damage, blood tests to detect diabetes or vitamin deficiencies. Imaging tests, such as CT or MRI scans, might be used to look for abnormalities, and finally nerve or skin biopsies could also be taken.
Treatment depends upon the causes of neuropathy. If the neuropathy was caused by vitamin deficiency, diabetes, infection, or toxic substances, addressing those conditions can lead to the nerve healing and sensation returning to the area. However if the nerve has died, then sensation may never come back to the area. Pain medication may be prescribed for less serious symptoms. Topical creams may also be tried to bring back sensation. Electrical nerve stimulation may be used for a period of time to stimulate nerves. Physical therapy can strengthen muscle and improve movement. Finally surgery might be necessary if pressure on the nerve is causing the neuropathy.
If you are experiencing sensation loss, numbness, tingling, or burning sensations in your feet, you may be experiencing neuropathy. Be sure to talk to a podiatrist to be diagnosed right away.
Peripheral neuropathy, a type of nerve damage that affects the extremities, is a complication associated with several diseases. One of the most common types of neuropathy is diabetic neuropathy. As its name suggests, this type of nerve damage occurs in people who have diabetes. Approximately 25% of diabetics have experienced pain caused by nerve damage. Other potential causes of peripheral neuropathy include vitamin deficiencies, alcohol abuse, foot injuries, hypothyroidism, kidney disease, Charcot-Marie-Tooth disease, and certain infections. Since neuropathy in the feet can cause a reduction or loss of sensation, the feet are at an increased risk of developing wounds, which may become infected. If you have peripheral neuropathy, it is suggested that you be under the care of a podiatrist.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with one of our podiatrists from Riznyk Podiatry. Our doctors will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our office located in Orchard Park, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Rheumatoid Arthritis is a chronic progressive disease that attacks several joints throughout the body. It is an autoimmune disease in which the body’s immune system mistakenly attacks the joints. As a result, the tissue inside the joints, called synovium, starts to thicken and causes pain around the joints. The synovium is responsible for creating a fluid that lubricates the joints to help them move. Approximately 1.5 million people in the United States have Rheumatoid Arthritis. Women are almost three times as likely to have RA compared to men, and it’s disease usually begins between the ages of 30 and 60. People who have a genetic history of RA are more likely to develop the disease.
Symptoms of RA may include the following sensations in the joints: pain, tenderness, swelling, redness, warmth, stiffness, and loss of range. Swollen joints are a very common symptom for those with the disease. At times, it may be minimal, but it may also be very apparent. Another typical symptom is joint stiffness. Doctors will often use the direction of morning stiffness to measure the severity of a patient’s joint inflammation. Other RA symptoms include limping, anemia, fever, and fatigue.
To diagnose RA, your podiatrist will typically request x-rays to see how much damage there is in the joints. Blood tests may also be performed to show if there are any signs of anemia, or antibodies such as the rheumatoid factor. If you have previously been diagnosed with RA, you should know the disease may spread to your feet and ankles.
There are many non-surgical options that can be used to treat this ailment. Some of these options include physical therapy, foot massages, orthotics, bracing, supportive shoes, and steroid injections. Physical therapy is useful because it will help stretch and strengthen the joints in both the foot and ankle to improve joint function. Massages can help improve blood circulation which will be good for the feet. Choosing proper footwear will allow you to walk with comfortability if you are a sufferer from RA. Lastly, bracing will help stabilize the foot joints, limit deformities and decrease pain.
In severe cases, surgery may be a treatment option that should be considered. For those who cannot walk without experiencing pain and those whose deformities can not be managed with braces, surgery should be considered. Your podiatrist will recommend surgery if he or she believes it will improve your foot biomechanics.
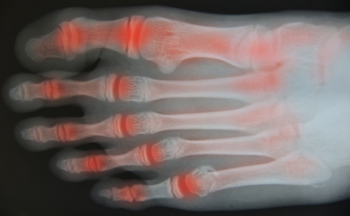 Rheumatoid arthritis (RA) is an autoimmune disease in which the body’s own immune system attacks and destroys otherwise healthy cells in the lining of the joints. There are several groups of joints in the lower limbs that are frequently affected by RA. The interphalangeal joints, which are located between the bones that make up the toes, and the metatarsophalangeal joints, which connect your toe bones to the rest of your foot, can become stiff, swollen, and inflamed. Hammertoes or claw toes may develop over time, keeping the toes bent at uncomfortable angles. The subtalar joint, located between the heel bone and the bone that connects your foot to your leg, and the ankle joints, can also become stiff, restricting the range of motion in your feet and ankles. If you have RA, it is suggested that you seek the ongoing care of a podiatrist.
Rheumatoid arthritis (RA) is an autoimmune disease in which the body’s own immune system attacks and destroys otherwise healthy cells in the lining of the joints. There are several groups of joints in the lower limbs that are frequently affected by RA. The interphalangeal joints, which are located between the bones that make up the toes, and the metatarsophalangeal joints, which connect your toe bones to the rest of your foot, can become stiff, swollen, and inflamed. Hammertoes or claw toes may develop over time, keeping the toes bent at uncomfortable angles. The subtalar joint, located between the heel bone and the bone that connects your foot to your leg, and the ankle joints, can also become stiff, restricting the range of motion in your feet and ankles. If you have RA, it is suggested that you seek the ongoing care of a podiatrist.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact one of our podiatrists of Riznyk Podiatry. Our doctors will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in Orchard Park, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Millions of people are affected by diabetes each year. Diabetes damages blood vessels in all parts of the body, especially the feet. The legs and feet may develop slow blood flow, which causes neuropathy, or nerve damage. Once a diabetic patient develops neuropathy, it is important that the feet are well taken care of. Otherwise, the lower limbs may have to be amputated. This only happens in drastic cases, but it shows how seriously diabetic foot care should be taken.
It is very important to always wash and dry the feet thoroughly, especially in between the toes, if you’re a diabetic. Secondly, examining your feet and toes for redness or sores must be done, even if you do not feel pain. You may also want to examine your feet from the bottom. Try to avoid wearing colored socks to prevent infections that may occur from the dye. Well-fitting socks are also highly recommended.
A diabetic’s physician should always monitor their blood levels to test how well blood sugars are being maintained. In addition to giving advice about everyday eating habits and foot care, a physician may prescribe medicine to help with the diabetic patient’s neuropathy. It is also advised to see a podiatrist if experiencing any feet conditions. Toenails may also need to be taken care of by a podiatrist. This prevents patients from cutting too deeply around their cuticles, which can lead to infection.
A person can take care of their feet at home by following the instructions of their physician. Using creams on one’s feet is also an effective way to heal dryness. Proceed with caution when using tools to remove calluses, as severe diabetics may not be able to feel pain on their feet. If any complications arise do not hesitate to contact a podiatrist.
On a daily basis, diabetic feet must be checked. If you are ever concerned about something, contact your health care professional. You never want to wait until a wound becomes too severe to treat. If left untreated, gangrene may develop. Gangrene is a serious infection that can lead to sepsis or amputation. It is also important for diabetics to be on the lookout for ulcers. Ulcers are sores that develop from tissue loss on the skin. They can be quite painful and require intensive treatment. Early treatment and everyday inspection are imperative to staying healthy.
 Because diabetes can bring with it other problems, particularly in your feet, it is a good idea to pay special attention to their care. Symptoms to watch out for include numbness, tingling, and a feeling of pins and needles. In addition, inability to feel hot or cold, discoloration, and pain or burning sensations are common. It is especially important to be aware of cuts that are slow to heal and cracks in the skin. Conditions that can result from neglecting your feet include foot ulcers, bacterial or fungal infections, and swelling. Some home remedies include washing and carefully drying your feet daily, applying moisturizer on them to prevent cracking, and always wearing shoes indoors. By far the most cautious approach to your foot care is to schedule regular visits with a podiatrist who can examine your feet and offer any treatment that becomes necessary.
Because diabetes can bring with it other problems, particularly in your feet, it is a good idea to pay special attention to their care. Symptoms to watch out for include numbness, tingling, and a feeling of pins and needles. In addition, inability to feel hot or cold, discoloration, and pain or burning sensations are common. It is especially important to be aware of cuts that are slow to heal and cracks in the skin. Conditions that can result from neglecting your feet include foot ulcers, bacterial or fungal infections, and swelling. Some home remedies include washing and carefully drying your feet daily, applying moisturizer on them to prevent cracking, and always wearing shoes indoors. By far the most cautious approach to your foot care is to schedule regular visits with a podiatrist who can examine your feet and offer any treatment that becomes necessary.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Riznyk Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Orchard Park, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
For hundreds of years, women have been wearing various kinds of high heels for aesthetic reasons. Women who wear high heels appear to be taller and have longer and thinner legs, and the wearer’s gait and posture changes. Though high heels have had an association with femininity and have kept them popular over the years, there are definite health problems caused by wearing them too frequently.
The motion of the ankle joints is limited when heels are worn. The ankle joint is very important to the body when it comes to walking. Because of their location, these joints have a great deal of weight put on them. Thus, it is very important to keep them as healthy as possible. The Achilles tendon is the main tendon in the ankle. Wearing high heels too often, studies have shown, can cause the calf muscle and Achilles tendon to shorten and stiffen. This can cause problems when shoes without heels are worn.
By putting a great deal of pressure on the ball of the foot and by forcing the toes into a small toe box, high heels can cause or may worsen many foot problems. These include corns, hammertoe, bunions, Morton’s neuroma and plantar fasciitis.
Not only does wearing high heels regularly have negative effects on the feet, the rest of the body can suffer as well. The knees, one of the most important joints in the entire body, can be affected by wearing high heels. High heels can cause the knees to stay bent all the time. Also, it can cause them to bend slightly inward as well. Doctors believe that women can suffer from osteoarthritis later in life because of constantly walking like in high heels. By limiting the natural motion of the foot during walking, high heels also cause an increased in stress on the knees.
Similarly, high heels can cause the back to go out of alignment. If high heels are worn constantly, the spine’s ability to absorb shock can cause continued back pain. They can compress the vertebrae of the lower back, and can overuse the back muscles.
However, this is not to say that high heels can never be worn. If worn occasionally and not often, they will not cause serious problems. They should not be worn every day. It’s important to wear them modestly to avoid the long-term physical health problems of the feet, knees, ankles, and back mentioned above.
In the ice, snow, and cold of winter, women frequently will wear boots rather than shoes. But some boots may be more dangerous than others. Boots with high or spiked heels and pointy toes may put the wearer more at risk on slippery surfaces. If your ankle rolls inward or outward, it could result in a fracture. Twisting your ankle can cause a sprain – a torn or stretched ligament. To avoid winter foot injuries, try low-heeled boots with traction soles, and avoid wearing high-heeled shoes outdoors. If you have fallen and hurt your foot or ankle, it is a good idea to make an appointment with a podiatrist who can examine the injured area and recommend options for treatment.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact one of our podiatrists from Riznyk Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
What Kinds of Foot Problems Can Develop from Wearing High Heels?
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our office located in Orchard Park, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.